In this category you'll find;
- Information that will help you before your surgery
- Leaving hospital and going home
- Discomfort and Pain
- Posture
- Exercises after your operation Day 1-7
- More advanced exercise after Day 7 onward (next page)
- Seroma
- Cording
- Altered Sensation in your armpit or arm
- Activity and lifting
- Lymphoedema
- Driving
- Feelings and emotions
DIEP and TRAM Breast Reconstructions
DIEP and TRAM flap reconstructions can be completed immediately following a mastectomy as part of the same surgery, or delayed following completion of all your treatment. Your surgeon will have chosen the option which is most suitable for you and your diagnosis.
What is my surgery?
Mastectomy is removal of the breast and may also involve surgery or sampling of lymph nodes.
A DIEP flap reconstruction (deep inferior epigastric perforator artery) is where an incision is made along your bikini line and a portion of skin, fat, and blood vessels is taken from the lower half of your tummy, moved up to your chest and formed into a breast shape. Your tummy button is also reshaped in this procedure.
A TRAM flap reconstruction (transverse rectus abdominis muscle) is where a portion of fat, skin, blood vessels, and muscle is taken from the lower part of your tummy, moved up to your chest and used to rebuild the breast. A mesh is used to cover the area where the muscle was removed from. Your tummy button is also reshaped in this procedure.
As these are classed as large surgeries, you will need to stay in hospital for 4-5 days. It may be useful to make any arrangements for this intended stay before your operation.
Information that will help you before your surgery
What to wear
Before you come into hospital for your operation think about the clothes you will wear in hospital and to go home in. Loose fitting clothing with front fastenings and trousers with a loose waist band may be easier and more comfortable to wear in the first few days following your operation. Consider what will be easy to get on your feet to walk in. Bring appropriate clothing in to hospital with you
A well supported, non-underwired, but comfortable bra is best. It would be ideal if it was front fastening, with adjustable straps, and be a bigger size to allow for any swelling. To reduce the risk of infection 2 bras would be appropriate, one to wash and one to wear.
Your consultant may advise that you wear a bra day and night initially.
![IMG_1356[1]](http://yoursurgeryandrehab.co.uk/wp-content/uploads/2017/05/IMG_13561-225x300.jpg)
Leaving hospital and going home
You must not drive yourself home from hospital so you must think about who will take you home after your operation. You must still wear a seatbelt as a passenger in a car. It may be more comfortable for you to use a small pillow to cushion the surgical area from the seatbelt for the journey home.
You may feel more confident to sit in the back of the car initially.

Discomfort and Pain
Discomfort, and some pain is common after any operation and you will be given a small supply of pain relief to take home with you. If you need additional or stronger pain relief you should contact your GP after your surgery.
- It is very important to take the pain relief that you have been prescribed regularly, especially in the first few weeks after your operation.
- Pain relief will allow you to move more freely and with less discomfort. It will help when you are completing your physiotherapy exercises in the day and can also give you a better night's sleep.
- Constipation is often a side effect of certain stronger pain relief. If constipation is a problem, drink plenty of fluids, make sure you have enough fibre in your diet, and consider using a gentle laxative available from the chemist.

After your Surgery
Breathing and Circulation Exercises
You will have been in surgery for some considerable time and so breathing and circulation exercises are important to keep your lungs clear, and reduce your risk of developing complications such as a chest infection or blood clots.
Practice breathing exercises
Relax your shoulders. Take 3-4 slow deep breaths in through your nose to fill your lungs as much as possible. If able, hold your breath for a couple of seconds and then try to sniff a bit more air in, before you then breathe out.
Supported cough: If you need to cough or sneeze, try to hold a pillow firmly over your stomach to support the wound. You can also try opening your mouth and forcing the air out hard, as if you are steaming up a mirror. This helps to bring any phlegm to the back of your throat. Don’t be scared to cough to clear any phlegm, you will not harm your wound.
You can start the breathing exercises as soon as you wake up. Try to practice every hour for the first 5 days or until you are up and walking regularly.
Circulation
As with the breathing exercises, it is vital you practice ankle exercises regularly. This helps to keep your circulation moving while you are more immobile and reduces the risk of a blood clots. This is until you are up and about and walking regularly. Remember also not to sit or lie with your legs crossed.
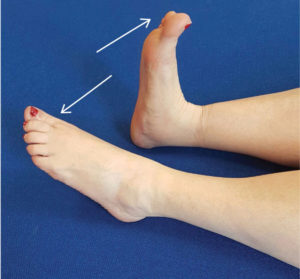
Practice paddling your feet up and down and circling from the ankle every hour 5 times.
Physiotherapy
A physiotherapist will come and see you the first day after your operation to explain the exercises. With assistance, you should aim to sit out of bed the first day after your operation and to start to walk short distances on the second day. Any discomfort or pain will be managed by the nursing team.
Positioning
After your operation, you will be positioned in bed with your hips and knees bent to avoid tension on your abdominal wound. Avoid pulling on the bed rails or pushing up using your affected arm. You are safe to lie on your side when it feels comfortable to do so.
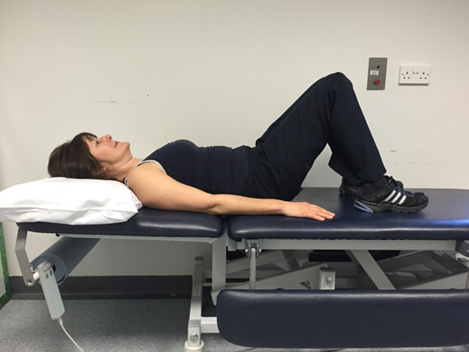
This is your position in bed
Sitting Try to correct your posture while you are sat in a chair, with your back supported and your shoulders level and relaxed. Avoid slumping. The physiotherapist or nurse will help you with this.
Standing When you first stand up and start walking you may find that you are unable to fully straighten up. Do not try to over-stretch your stomach wound initially. About a week after your operation you should be walking more upright.
When walking, allow your arms to fall naturally by your sides and try not to hold your arms bent in front of you.
Getting out of bed
For the first 6 weeks after your operation, you should aim to use a “log roll” technique to get in and out of bed. This will help reduce pain and stress on your abdominal wound. You will need help with this for the first few days.
Log Roll Technique
- Lying on your back, bend your knees so your feet are flat on the bed
- Slowly roll your body onto your good side (the side that has not had surgery)
- Slide your legs off the side of the bed
- Gently push yourself up into a sitting position with your good arm (the arm that has not had surgery)
Reverse the procedure when getting into bed.
Exercises for days 1 - 7
Click here for information, images and videos
Exercises for days 7 onwards
Click here for more information, images and videos
Drains
You are likely to have a surgical drain in following surgery to collect any excess fluid. Sometimes all the drains are removed on the ward, however it is not unusual to go home with a drain.
Here are some tips for going home with drains.
- You are safe to walk with drains in. It may be useful to carry them in a light shoulder bag or plastic bags for ease.
- Try additional pillows at home to help you find a comfortable position during the day and at night.
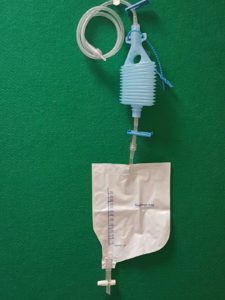
- You should not lift your elbow above your shoulder height whilst drains are in. You can still reach your head to brush your hair and should complete the first physiotherapy exercises (Days 1-7) as normal.
- Keep a record of how much is drained every 24 hours, and bring this record to your next clinic appointment.
- Your drain/ drains will be removed in clinic. Allow your arm to rest following drain removal and do not complete your physiotherapy exercises for the rest of that day. Start back with your exercises the following day.
Seroma
It is common to experience swelling around your surgical site or in your armpit after your surgery. This is a natural collection of fluid called a Seroma which the body will gradually reabsorb over time.
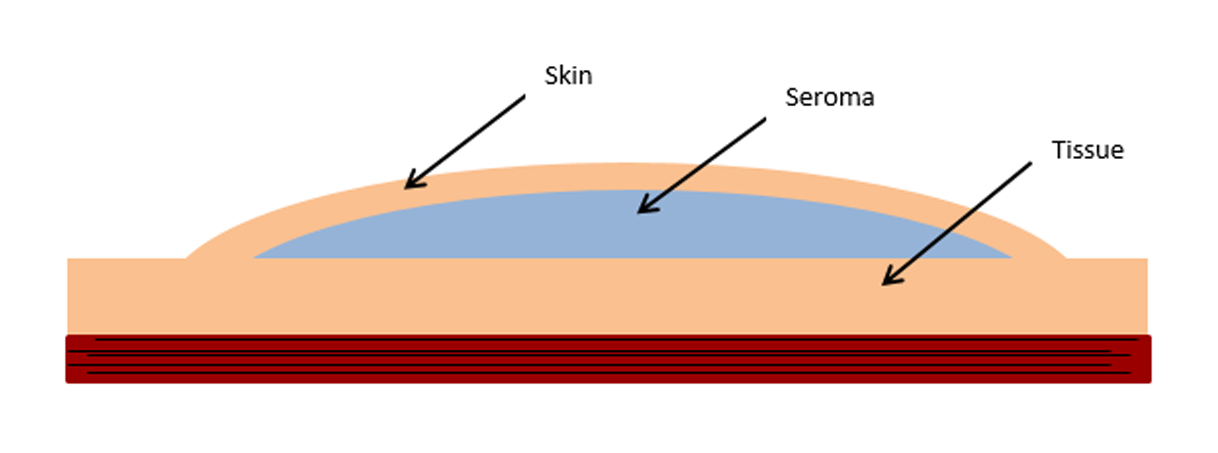
A seroma is not harmful but occasionally becomes very uncomfortable or puts too much pressure on the new wound. If this happens, you will need to contact the plastics dressings clinic or ward F1 South (evenings, weekends and bank holidays) to have this excess fluid drained.
This is a small painless procedure which may have to be done more than once during your recovery.If you have had a seroma drained, please leave your physiotherapy exercises for the rest of that day to prevent the seroma refilling. Start back with your exercises the following day.

Posture
It is very important to look after your posture following your operation. It is common to feel that you need to be protective of your wounds however, it is vital to try and sit, stand and walk normally. This will help you avoid getting stiffness in your shoulder, neck and elbow and limit any future problems.
This is poor shoulder posture.
Here is a really simple exercise to help your posture. Try this little and often during the day.
Posture Correction Exercise
- Stand tall, imagining you have a string pulling you up from the middle of your head.
- Gently lower your shoulders down towards the floor.
- Gently take your shoulders backwards, bringing your shoulder blades together.
- Hold for 5 seconds then relax. Try to complete this 10 times.
Altered Sensation
After your surgery, you may notice numbness to your new breasts and stomach area. This is a normal sensation that occurs as a result of nerves being temporarily damaged during surgery.
These sensations will settle with time but this may take weeks and months. You may have some areas which will always remain numb.
If you are concerned speak to your surgeon at your next clinic appointment.
Activity and lifting
It is normal to feel tired and low in energy during your first few weeks at home. However we would encourage you to do small amounts of activity as you feel able.
You should aim to get up and move around regularly in the day, but also have regular periods of rest. Initially, you may need a small amount of support to be able to wash and dress yourself and complete personal hygiene. By 2 weeks after surgery, you will be able to perform these tasks independently however they may take you longer than usual.
![IMG_1338[1]](http://yoursurgeryandrehab.co.uk/wp-content/uploads/2017/05/IMG_13381-300x225.jpg)
By 2-3 weeks after surgery, you will be able to complete light household tasks and washing up by yourself, but don’t try to lift anything too heavy with your affected arm.
For the first 2- 3 weeks please do not carry or lift anything heavier than a bag of sugar (approximately 2 lbs/ 1kg) and only carry these items for a maximum of 5 minutes
If you are responsible for the care of someone else you will need to make arrangements for help with this whilst you recover from your surgery. Please speak to the ward staff if you are struggling with this.

For the first 8-12 weeks avoid heavy and repetitive tasks such as
- Sweeping
- Mopping
- Ironing
- Changing duvets
- Moving wheelie bins
- Pushing/ pulling activities
The return to your usual activities is a gradual process and it is important to pace yourself. You may have some shoulder or tummy discomfort as you rebuild your strength but if your arm or tummy starts to ache you should stop, have a rest, and go back to the activity later. Listen to your body!
Gradually increase your activity levels but do not attempt to lift heavy objects such as shopping, vacuums, watering cans for 4 months following your surgery.
When you do lift, (even light objects), take care with technique. Keep your feet apart, bend your knees, keep your back straight, engage your stomach muscles, hold the object close to your body and straighten from your knees.
Walking is an excellent way to gently re-build your fitness levels whether it’s indoors or outdoors . Try to include walking into your daily routine. Be aware of your energy levels though and dont go too far. Plan to gradually walk further as you feel able.
You will be given advice on returning to leisure activities and sport as part of your rehabilitation class.
Lymphoedema
Lymph is a normal colourless fluid that occurs in the body, in a system of lymph vessels and lymph nodes often called glands. Some patients may develop a persistent swelling of the arm and/ or breast following removal of lymph nodes in the armpit and this is called Lymphoedema.
If you have previously had lymph nodes removed or have lymphoedema already you may notice some increased swelling in your arm or hand after this surgery. This is not unusual and should settle over the first 3-4 weeks. Please contact your lymphoedema team if you require support or a change in your compression garment
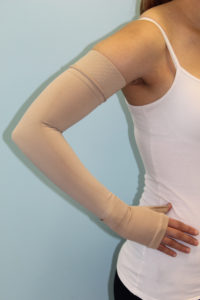
Lymphoedema may continue to be a risk, however, there are some sensible precautions that you can take. You will be given these precautions in your rehabilitation class, as well as full instruction on skin care, scar massage, hair removal, dos and don’ts and exercise which can help reduce your risk.
Driving
You are advised not to start driving for at least 6 weeks after your surgery. Healing and strengthening needs to happen before you are safe to drive.
When you do start to drive you will need to make sure you have good arm movement and be sure that you can control the vehicle. This includes repetitive gear changes, braking, using the handbrake and being able to react in an emergency. Start with a small journey and gradually increase the distance as you feel stronger.
You are advised to contact your insurance provider to ensure you are covered following your surgery.

Feelings and emotions
Remember this reconstruction is work in progress. At this early stage you will have normal swelling and bruising after your surgery and this will take time to settle. This will affect how your reconstruction looks and is not your final outcome. Please talk to your plastics team if you have any concerns.
You can find additional support available on the website and you will be directed to support in your local area at the rehabilitation class.
Should you have any concerns or worries about your exercises please contact the physiotherapists at the Nightingale Centre on 0161 291 4268.
You will attend a one off instruction class 6-8 weeks after your surgery as part of your continuing treatment. At this class, you will be shown your follow-on physiotherapy exercises, and be given advice on activity and exercise now and in the future. There is also information and advice on skin care, scars, cording, diet and how to reduce your risk of Lymphoedema. This session is an opportunity for you to ask questions of the rehabilitation team and learn how to access local services in the Manchester area.